Government of India launched world's largest healthcare insurance scheme Ayushman Bharat Pradhan Mantri Jan Arogya Yojana (PM-JAY) in 2018. And, by October 2025, more than 42,17,58,675 Ayushman Cards have already been issued and over 10,40,33,937 hospital treatments have been provided worth nearly ₹1.3 lakh crore. The scheme provides a free health insurance cover of ₹5 lakh per family per year and is known as the world’s biggest government health scheme.
Since its launch in 2018, Ayushman Bharat Yojana has helped crores of families get free hospital treatment across India. The government continues to expand the scheme every year so that no poor or middle-income family has to face money problems due to medical costs. All citizens above 70 years, ASHA and Anganwadi workers, and millions of poor families are now included under this scheme. The registration process has also become easier with full online facilities.
What is Ayushman Bharat Yojana?
Ayushman Bharat Yojana, also known as PM Jan Arogya Yojana (PM-JAY), is a national health protection scheme started by the Government of India in 2018. It offers cashless treatment up to ₹5 lakh per family per year in both government and private hospitals that are part of the scheme.
This means that if any member of the eligible family needs hospitalization for surgery, therapy, or any major disease, the hospital bill will be paid by the government. You do not have to spend any money from your pocket. The treatment is paperless and completely cashless. The scheme aims to help poor and middle-class families who earlier struggled to afford good medical care.
Quick Highlights
| Scheme Name | Ayushman Bharat – Pradhan Mantri Jan Arogya Yojana (PM-JAY) |
| Launched On | 23 September 2018 |
| Implemented By | National Health Authority (NHA), Government of India |
| Annual Health Cover | ₹5 lakh per family for secondary and tertiary hospital care |
| Families Covered (2025) | Over 15 crore families (80+ crore people) |
| Empaneled Hospitals | 32,000+ public and private hospitals across India |
| Beneficiary Cost | Free - 100% government funded |
| Special Coverage | ₹5 lakh extra cover for citizens above 70 years (Ayushman Vaya Vandana) |
| Helpline Number | 14555 (toll-free, 24x7) |
| Official Website | pmjay.gov.in |
Eligibility for Ayushman Bharat Yojana
Ayushman Bharat Yojana is meant for poor and at-risk families based on the Socio-Economic Caste Census (SECC) 2011. You don’t have to apply separately if your family is already listed in the official beneficiary database. The eligibility rules differ slightly for rural and urban families.
Rural Areas Eligibility
- Families living in one-room kucha houses
- Households with no adult earning member
- Scheduled Caste (SC) / Scheduled Tribe (ST) families
- Families with disabled members and no adult support
- Landless laborers depending on daily wages
Urban Areas Eligibility
- Ragpickers, beggars, domestic workers, street vendors, construction workers, plumbers, drivers, shop helpers, and similar occupations
There is no age limit or family size restriction. Everyone in the eligible family, from newborns to grandparents, is covered. In 2024 - 25, the government added ASHA and Anganwadi workers and all citizens above 70 years under this scheme. Senior citizens get an additional ₹5 lakh health cover through the Ayushman Vaya Vandana Card.
Check Ayushman Bharat Eligibility Online
You can check the eligibility for Ayushman Bharat Yojana coverage at the official portal by visiting pmjay.gov.in and click on "Am I Eligible" and then login using mobile number and enter details such as you Aadhaar number, state & district to check your eligibility for the scheme.
You can also call the toll-free number 14555.
Benefits of Ayushman Bharat Yojana
Ayushman Bharat Yojana offers several strong benefits that make it one of the best healthcare schemes for Indians. Here are the main features:
- ₹5 Lakh Free Health Cover: Each family gets ₹5,00,000 per year for hospitalization expenses. The amount can be used by any family member as needed.
- Cashless and Paperless: No need to pay or submit forms at the hospital. The bill is settled directly between the hospital and the government.
- All Major Treatments Covered: More than 1,500 medical and surgical procedures across 24 specialties are included, from heart and kidney surgeries to cancer and maternity care.
- Pre and Post-Hospitalization Costs: Expenses up to 3 days before and 15 days after hospitalization are included in the package.
- Nationwide Portability: The Ayushman Card can be used anywhere in India, whether you live in a village or another state.
- All Ages and Family Sizes Covered: There is no limit on the number of family members or their ages.
- No Premium or Hidden Charges: It’s totally free for the beneficiary; the government bears the entire cost.
Documents Required for Ayushman Bharat Card
- Aadhaar Card: Mandatory for identity verification through OTP or biometric.
- Ration Card or Family ID: Useful to confirm family members linked to your household.
- Mobile Number: Required for OTP verification and status updates.
- Passport-size Photo: Optional, for printed cards.
There is no income proof or caste certificate needed in most cases. If your family is already listed as eligible in the government database, Aadhaar is usually enough to complete the verification.
How to Apply Online for Ayushman Bharat Card (PM-JAY Card)
You can apply yourself on the official website using the below steps or visit a nearby Common Service Centre (CSC).
STEP 1: Visit the official website pmjay.gov.in and click on the "Am I Eligible" option.
STEP 2: Enter your mobile number and captcha code, then click on Generate OTP. Verify the OTP received on your phone to log in.
STEP 3: Select your state and search your family details using your name, ration card, or Aadhaar number. If your name appears, click on it to start eKYC verification.
STEP 4: Choose Aadhaar OTP method for eKYC verification. You will receive another OTP on your Aadhaar-linked mobile number. Enter it to verify your identity.
STEP 5: After successful verification, wait for about 10 - 15 minutes. Then log in again at beneficiary.nha.gov.in to download your Ayushman Bharat Card PDF. This is your official e-card containing your name, ID, and QR code.
If you find this process difficult, visit your nearest Common Service Centre (CSC) or an Ayushman Mitra desk at any government hospital. They will help you generate and print your card instantly, free of cost (only ₹30 may be charged for PVC printing if requested).
How to Check Ayushman Bharat Hospital List Online?
To get treatment under Ayushman Bharat, you need to visit a hospital that is part of the PM-JAY network. Here’s how to check which hospitals are included:
STEP 1: Visit Hospital search website of NHA at https://hem.nha.gov.in/search.
STEP 2: Choose any of the options from by pin code, district, facility name or advance search.
STEP 3: Choose your State and District from the dropdown menu or enter your PIN code.
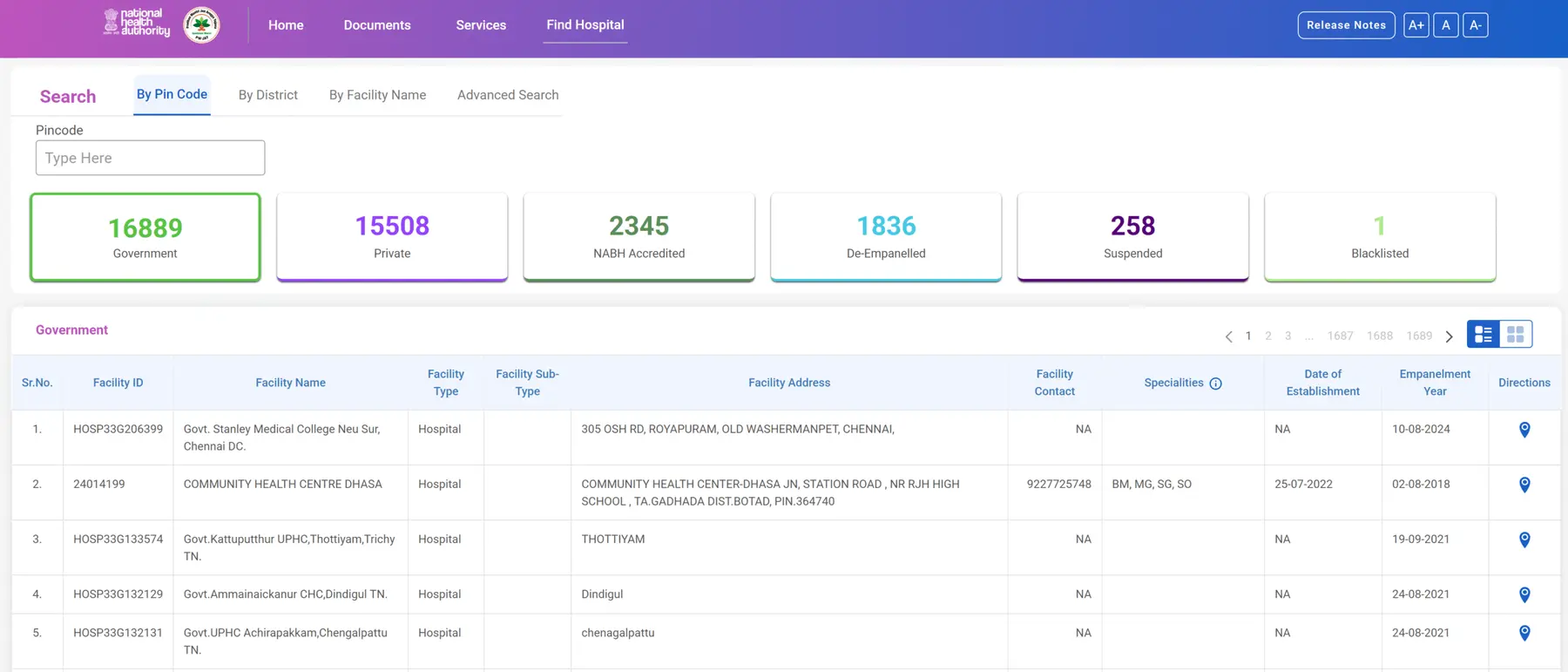
STEP 4: You’ll see a list of all public and private hospitals under PM-JAY in your area. You can also download the full hospital list PDF from the site for offline use.
The hospital network now includes over 32,000 facilities across India. Each empanelled hospital displays the PM-JAY logo or "Ayushman Bharat Accepted Here" board at the entrance.
How to Download Ayushman Bharat Treatment Packages List?
National Health Authority publishes a detailed list of all treatments covered under Ayushman Bharat, known as the Health Benefit Packages (HBP). This list includes package names, codes, and government-approved rates.
STEP 1: Visit the official National Health Authority website: nha.gov.in.
STEP 2: Go to the "Packages and Rates" section and click "See Health Benefit Packages".
STEP 3: Download the latest HBP PDF file. It contains all procedures and rates.

STEP 4: Open the PDF and search for your treatment (e.g., "Dialysis", "Heart Surgery", "C-Section") using the find option.
The package list covers about 1,500+ procedures, including all major treatments like kidney transplant, heart bypass, cancer therapy, maternity care, orthopedics, and ICU services. The rates are fixed, so hospitals can't charge extra. You can check these details anytime to know what is included in your free coverage.
Helpline and Support
For any issue related to Ayushman Bharat Card or hospital treatment, you can call the official toll-free helpline 14555. It’s available 24x7 in multiple languages. Alternate numbers are 1800-111-565 and 1800-11-0770.
Guidelines for Hospitals and Patients
For Hospitals: All empanelled hospitals must provide cashless treatment to Ayushman beneficiaries. They cannot charge extra money for covered treatments. Hospitals must follow fixed package rates and upload treatment details online. Misuse or overcharging can lead to removal from the network.
For Patients: Always carry your Ayushman Card or Aadhaar when visiting the hospital. Visit only empanelled hospitals, and do not pay any amount for covered services. If a hospital denies treatment, immediately call 14555. Treatment under this scheme is completely free, including medicines, tests, ICU, and surgeries.
Latest Updates and Statistics (2024 - 2025)
Ayushman Bharat Yojana has grown fast in the last two years, making it truly a nationwide health protection program.
- New Coverage for Senior Citizens: From 2024, all citizens aged 70+ are eligible for an additional ₹5 lakh cover under the "Ayushman Vaya Vandana Card".
- ASHA & Anganwadi Workers Included: Around 37 lakh families of front-line health workers added in 2024.
- Almost All India Covered: 35 of 36 states and UTs now implement PM-JAY; only West Bengal runs its own scheme.
- Families Covered: 15.1 crore families (over 80 crore people) have been included.
- Hospital Network: 32,000+ empanelled hospitals.
- Treatments Provided: Over 10 crore hospitalizations worth ₹1.4 lakh crore completed.
- Digital Integration: 94% cards linked with Aadhaar and more than 76 crore digital ABHA health IDs created.
- Union Budget 2025-26: ₹9,406 crore allocated for PM-JAY scheme.
Most beneficiaries (82%) belong to rural India, showing the success of the scheme in reaching the poorest households. Dialysis and maternity care remain among the top treatments availed by people under PM-JAY.
FAQs
Who is eligible for Ayushman Bharat Yojana?
Families listed under SECC 2011 in rural or urban poor categories are eligible. Also, ASHA/Anganwadi workers and all citizens aged 70+ can apply irrespective of income.
How can I apply for Ayushman Card?
Visit pmjay.gov.in, click "Am I Eligible", verify with mobile OTP and Aadhaar, and download your card after eKYC. You can also visit a CSC or Ayushman Mitra desk for offline help.
What benefits do I get?
Free hospital treatment up to ₹5 lakh per year for the whole family covering 1,500+ diseases, including heart, cancer, kidney, and maternity care. The entire process is cashless.
Are there any fees?
No. The card and all services are completely free for eligible families. Only ₹30 may be charged for optional PVC printing at a CSC.
What if the hospital denies treatment?
Immediately call 14555 or inform the Ayushman Mitra at the hospital. The hospital is not allowed to refuse treatment to any verified beneficiary.


My name is Mohammad Gulab
Joint me
Ineed home loans
hi mu name is shravan kumar sharma
10+2 vill+post rohana sardaspur dist-ballia
can you give me job sir
hello sir good evening
i am Nidhi Prajapati
i am heart paisent.my family is very poor.....so please help me.
thanks you
I need health insurance
join me
pls join me
Job
hi may dilip khatik hu mare papa bimer h paysi ko jarurat h plz give mi halp
Job
VERY GOOD.
is RSBY/ SSK card covered under the Bhart Ayushman progman ?
very good
very good budget
National health protection is good job
good scheme for all indian
Manoyar sekh raihan sekh Gile ajmira ajmoddin younus sekh kanutia birbhum pin no731213
How could,we APPLY in NHPS
This scheme will provide medical insurance cards to every person and will start from 15 August 2018 or 2nd October
BUT WHAT! ALL medical PROCEDURES will be covered BY Any Insurance Scheme: Will Blood Transfusion (Rs 10,000) for the anemic; Sodium Saline Drip for LOW sodium Patients (Rs 3000-4000)>>?? pramodkaimalatgmail ha ha ha
The central scheme for medical facilities and support is fine. Health care clinics should be organized by NGOs.
We will work on it
Good job sir
20.00000
Under Prime Minister's Swastya Beema Yojana
Blood Transfusion for Elderly 85+ years OLD is NOT included NOW
SO it cost me Rs 7000 (seven THOUSAND) plus to get the Transfusion for my 87 year old Father when His Hemoglobin COUNT went down to 5 and he got Breathless with Palpitations (He got Anemic)
Also it cost Rs 3000 WHEN HIS SODIUM WENT LOW and he fainted on the ROAD and had to be given Saline for 3 days till the Sodium Level Stabilized
Thank YOU my Heart felt Thanks that Cataract is Included for a Cost up to Rs 9000 one eye . At a time (then 3 years or so later for other eye)
NOW may take for my 78+ Mother's Left eye (the rigfh eye was already treated for Cataract Removal at a Police Arranged Camp to be conducted at a Missionary Hospital for FREE (rigid lens) NOT flexible that which would set the cost go up to Rs 15000 (one eye)
Dandwath PRANAM 9496872890
Pramod Purushotham Kaimal
(Uniquely
Sri Atmanda Memorial school
Malakkara P.O.
Between Edayaranmulla and Chengannur
Pathanamthitta District
Kerala, Bharat 689532
A unique SCHOOL with THE UNIQUE APPROACH TO EDUCATION worth ONE STUDY VISIT by EDUCATIONISTS across the world
Namaste
Kindly Add medical procedures covered Under Swasthya Beema Yojana
[1] Blood Transfusion (for Anemic whose Blood Hemoglobin Count reach 5) Rs 9000+
[2] Saline DRIP till Sodium (Na) Level Stabilises for Lowering of Sodium and fainting
[3] If Possible INCREASE cataract Operation cost cover to Rs 15000 to be able to USE flexible Lens with Laser procedure
pranaams pramodkaimalatgmail 9496872890
what will be the EMI for this scheme?
EMI for this scheme is NIL (Rs. 0). Govt. will pay all the premium amount under this Health Insurance Scheme
AH-NHSM STILL IN BHARAT NO HOSPITAL ARE AVAILABLE. HOSPITALS ARE NOT MANAGED IN GOOD ENVIRONMENT AND HYGENIC. DOCTORS ARE LESS IN BHARAT. AGE FACTOR OF BHARTIYA AVERAGE 55 AS PER MY KNOWLEDGE. BHARAT HIGH POPULATED AREA DUE TO CASTE AND REILGION. POPULATION PROJECT OF INDIA LOST ITS FAITH. I BUILT PPP PROJECT BUILDINGS IN KARNATAKA 20 YEARS BACK ARE THEY DELIAPALATED.
I SUGGEST 24X7 DUTY BOUND HOSPITALS NEED FOR BHARAT.
WITHIN PERIMETER OF 2 KM WITH GOOD ACCESS OF ROAD IN THE INTENSILY POPULATED AREA OF 150 BEDEED HOSPITAL NEED BY GOI.
PRIVATE HOSPITALS TAKE TECHNOLOGY FROM ABRAOD WE GOI GOK WILL TAKE HIGH TECH MACHINES AND GOOD KNOWLEDGE DOCTORS TO MISSION SUCCESSSFUL.
rampur
scheme yearly fee not mention. half information given. IAS officers should know this. but i think they are not serious when they put it on cloud
where to apply for ayushman bharat
Kamalbhati3219@gmail.com
Kamalsingh Bhadli Jaisalmer RajsthanIn
VERY THANK FULL TO MR.PM NARENDRA MODI JI TO THIS GOOD PROJECT . MANU FAMILIES IN INDIA ARE NOT AFFORDABLE FOR MEDICAL EXPENSES. SO THIS WORK WILL BE VERY USEFULL .
Is it chargible for the citizen.
If yes how much?
No, the entire premium will be borne by the central and the state government. This scheme is entirely free for all citizens and thus will serve the poor people to a great extent.
Is this insurance coverage available for NHM contractual staff also, or u have criteria like BPL, SC ST ?????
Sir plz make availability of applications forms as soon as possible... Still now especially my family members did not got any nice advantage from your govt as no one in our family is having government jobs
We are working towards the complete roll-out of Ayushman Bharat Yojana 2018 as soon as possible.
** Share your comments & discuss with other community members on Sarkari Yojana Forums forums.sarkariyojana.com
PMAY KA UPEYOK kecha Karu p.H
Rajai Khera post Patari distic unnao
ISKE LIYE APPLY KAISE KARE
Sk8641342@gmail.com siwan
Sarkari hospital siwan m.9813053953
मैं भी यहीं कहुँगा, " ये योजना वास्तव में बहुत ही अच्छा और आज देश की स्थिति अनुसार आवश्यक भी हैं। " सरकार को जरुरी कदम के साथ जरूरतमंद लोगों तक पहुँचा कर इस योजना को सफ़ल बनाना चाहिए। जिसकी सफ़लता सामाजिक स्तर पर एक ऐतिहासिक जीत होगी।
!! धन्यवाद !!
ieggrythisbenifit
Sir want this policy me&my family how to apply
As soon as the 2nd component of Ayushman Bharat Yojana i.e issuing of Health Cards will start, we will update the complete application procedure here. It may be around 15 August 2018.
** Share your comments & discuss with other community members on Sarkari Yojana Forums forums.sarkariyojana.com
padhae ke liy lon
padhae ke liy lon berogari ke liy
Dear Sir,
I am Ratan Chakraborty aged about 65 years.Is a senior citizen want to apply my self for P.M Ayusman Bharat health insrance scheam.I have retaited from my service in 1995. In where no pension no others
employees benifit schehe.i am a lower middle class family in today my monthly income is 5000/-p.m.This
is my earnest request to you kindly send me a format for application for above scheme at the earliest &
oblige.
Thanking You,
Yours Faithfully,
RATAN CHAKRABORTY
26,DEBINAGAR<BAGPOTA ROAD,
SARSUNA,KOLKATA-700 061
PM Modi is going to launch this Ayushman Bharat Yojana 2018 Scheme on 15 August 2018. As soon as the Ayushman Bharat Registration Form will be available, we will update it here.
Achchi Yojana h
Under health account scheme we are giving health diaries to take care of citizens with the provision of once a month contact and updating on health-related all aspects- treatment tests, expense, and experiences. Lack of education and information can be done by one to one contact only as during baseline survey done under health account scheme only 3 % were found having access to the internet.
Sheela ms 95 Ramamandira road yaraganahalli mysuru 570011 mob9663190023 please sir nanage gudisalukuda illa sir
Sheela ms 95 Ramamandira road yaraganahalli mysuru 570011 mob9663190023 please sir nanage gudisalukuda illa sir
Sir can middle Class family apply for this health scheme And how to apply like Application forms and procedure. Pl. HELP.
Very good program,but what is the qualification for that training
It's great job for unemployed youth for India.
Sir you have given so much information that readiness was lost
sir me bhi ayushman mitra ka course krna chahta hu kese hoga ..frome kese apply kre
we appreciate the government for creating the job but salary is disappointed .salary must be 25000 INR for better life.
Rath road Indra Nagar orai Jalaun Uttar Pradesh
we appreclate the govemment for creating the job salary is must be 25000inr FOR BETTER LIFE
How i can Applay for this
VILL-MURHADI (B.T)POST+PS- BABUBARHI DIST-MADHUBANI STATE-BIHAR PIN CODE 847224
VILL-MURHADI (B.T)POST+PS-BABUBARHI DIST-MADHUBANI PINCODE-847224 STATE-BIHAR
Good but not fast as required
SIR MARA PAS APNA KOI MAKAN NAHI HAI MARE PITAJI KA MAKAN HAI HUM TIN BHAI HAI SABKI SADI HO GAI HAI KIYA ME AWAS YOJNA KE MADYAM SE MAKHAN BANBA SAKTA HU MARE PAS GARIBI RASAN CARD NAHI HAI MUJE IS YOJNA KA LAVA KASE MIL SAKTA HAI KRPIYA BATAYE
I want a ayushman Bharat center I have csc center
Sir
this is not implemented in punjab.. because punjab goverment refused to implement this ..
i have confirmed from CSC head in Punjab Mr. Jaspal Singh
What are the eligibility conditions? Ex servicemen are eligible or not? Duration of services? Please answer.
What are the eligibility condition. Age bar. Ex servicemen are eligible. Duration of services.
It will be very good health scheme,be spread and available at all corners and remotes of the country so that the needy people get their needed service in need at their door steps
what to do give me some massage
sir i m interested to this scheme as a csc how to open csc centre?
Good, I have join.
Kya BPL family ke liya koi health insurance h
I am kishor i am intreasted your Ayushman bharat yojana helth insuran....
My name is vishavmohan
it's great job for unemployed youth for india
new vidio aushaman mitra apply proses
The scheme announced very good but departmental employees are not good so poor people can not get scheme benefit
Pradip kumar
baibaha
bidhoona
auraiya up
206249
very good information. thanks for sharing your information..
jan arogya abhiyan ke liye kya qualification chaiea r ye kis state me kaise kya kam hoga iski form kb tk bhre jayenge please c9nvience me
Shakshi Sharma, if your name appears in the SECC 2011 Data (All India Final BPL List), which is the only qualification, then you can avail benefits of Health Insurance of upto Rs. 5 lakh. This PM Jan Arogya Abhiyan (Ayushman Bharat Yojana) will be launched on 25 September 2018 on birth anniversary of Pt. Deendayal Upadhyaya as told by the PM Modi on 15 August 2018 from Red Fort. Some states launch this scheme by merging their own state's health insurance scheme with Ayushman Bharat while some states will launch this scheme as it is.
jan arogya abhiyan ke liye kya qualification chaiea r ye kis state me kaise kya kam hoga iski form kb tk bhre jayenge please convience me
MAHARASHTRA ME KABSE LAGU RAHEGA
This AB-NHPS has to be applicable for all sr.citizens and not as per SECC-2011.
how to apply
Bhut badiya sir
Complete Information......Thanks
Bhut vadiya ji
Good
Thank You Sir
Please let me know details about PMJAY
Good step for all the poor people in India.please give me contact number for your helpdesk.
Excellent Initiative by our Honourable PM to the people who are in need .
please please help me
Ayushman bharat yojna bharat sarkar ki bahut hi sarahniy yojna hai yah yojna secc data ke gareeb pariwaro ko rojgar dekar unki aarthik sthiti majboot karegi pm narendra modi ji aapko dhanyabad
VILLAGE CHARHIYA P.O SEMRA MEDROL P.S SEMRA BAZAR DISTIC WEST CHAMPARN BIHAR PIN NO 845105
I am interested to apply the post of ayushman mitra at Ranchi jharkhand 834001
i wish to empanel my multispeciality hospital with ayushman yojana.
Ayushman mitra job vacancy all update
Sar ba camepet hay koi jop ho to esa namber par pone kar dena 7355907474
Nice
when one can apply for the post aayushman mitra .
Mera name ramkumari vishwkarma h Meri age 19 h or me 12th pass hu call center me Job karti hu par mere heart me chhed bataye h hospital me Kya mujhe is yojna ka lav milega milega to mujhe kese apply karna h please please me abhi jina chahti mere mammi ke liye mujhe bohut kuch karna h please please please
my ayushaman service ma job karva babat
SIR. HAM IS JOJONAKE BAREME JANNA CHATEHE.
SIR, Excellent Initiative by our Honourable PM to the people who are in need
7 when will come vacancy of ayushman mitra in bihar please informe me at no.7011276892
when will come vacancy in bihar
me is yujna ka hissa hona chahti hu sr ji
how to apply
Now it is September. When will you release online application forms
Dear Respected sir.
Humhare Desh ke Manniya Pradhan Mantri Shri Narendra Modi ji ki es yojna me hum apna yogdan dekar desh ke sabhi nagriko ko labh dilana or sahyog karna chahte hai
Sy899728@gamil.com villege rupachandpur cholapur varanasi
sir pardhan mantri jan arogya yojna me kese jude sir please hel me
Please let me know details about PMJAY
very very good yogna hai
many many poorperson will be helpfull this yogna
I like modee
Good very good .I appreciate to Mr Narendra Modi PM Sir.
My husband, S S Rao served National Seeds Corporation Ltd for 28 years and took VRS in 1993. He is not entitled for pension or even medical facility. We don't have any assured source of income and dependent on children. Whether we can avail this Scheme or not? If so, please let us know about procedural formalities.
ABV Vijayalakshmi
Sr. Citizen, 75 years
Noida
N
Super modiji. thank you modiji
I KNOW TO PACKAGE LIST FOR AYUSMAN BHARAT
Super Modiji. thank you Modiji
Iam interested toapply the post of ayushman mitra at vp. Kemla Teh. Nadoti Dist.Karoli Rajasthan 322220
I LICK VERY GOOD MODIJI
kamlesh
I AM U.S.KANOJIA (UMA SHANKAR KANOJIA) I HAVE A PROBLEM IN MY RITE KNEE & UNABLE TO MOVE & WALK & CAN I ELIGIBLE TO GET THIS BENIFIT.
Nice sir this is a nice scheme
klvcmk.
હું આ યોજાના લોન્ચ કરવા બદલ તમારો ખુબ ખુબ આભાર માનું છું અને આ દેશ ના લોકો નો જીવન-ધોરણ ઊંચા આવે અને આપણે વિકસિત દેશો કરતાં પણ સારું આરોગ્ય રહે તે માટે નું આ પેલું પગથિયું છે અને આવી રીતે આપણે તેમના ક્રતા લાબું અને શારું જીવન જીવવા મા આ યોજના આ આપને ખૂબ મદદ કરશે
લી. પરેશ માળી
Very very good sir this scheme very useful benefeticaly poor familis god gift pm moodi sir 100 years pleauss sir neenga nalla ierukkanum sir......
Bhot achi Yojana ha Humare PL Modi Sir ki ma is ma kam krna chayti hu ... Sewa krna chayti hu..plz full info. dijiye ma foam fill kr sko
बहुत बढीया
मेरा लिस्ट मे नाम नही है
1 ) Lower Middle class : Less than 5.00 lakhs
2) Middle Class : Between 5.00 to 12.50 Lakhs
3) Upper Middle Class : Between 1250 lakhs to 20.00 lakhs.
It is extremely disheartening and sad that Lower Middle Class and Lower of the Middle class
i.e. Between 5.00 to 7.50 lakhs beaten by Taxes from 360 degrees , ever increasing inflation and Low interest on Bank savings and No Job Opportunities for their children find Living difficult in this country. Here I am not against BPL families at all as this class up to 7.50 lakhs is closely aligned to BPL families economically as OBCs to SC/ST class. Here since Medical cover is for Family ( Spouse and Children and dependent parents ) I have taken total family income in above gradation and not individual income alone, may be noted. On behalf of my late learned father who suffered paralysis and my Bed-ridden mother , I convey blessings to Hon'ble Prime Minister Shri Narendra Modiji and Hearty congratulations to Health ministry. I request Health ministry to carry this message and keep on P.M.s table which would give him all inspiration and boost his moral strength to do Justice to economically depressed middle class also wherein he himself has continuously struggled and suffocated to reach the present illustrious and glorious office. My Warmest regards to him.
........ V.N. Phadnis ( M : 94489 21263 )
supper pm sar
pm arogya yojana variy poor ga unna vari kaniru thudichpattuthnndi sar thanks
why this scheme is not implemented in telugu states?
vill.post.ps sursang dist gumla (jharkhand)
Pin no. 835232
vill.post.ps sursang dist gumla (jharkhand)
Pin no. 835232
How to get the list of hospitals which are providing cashless treatment Under this great initiative?
My mother got admitted in a private hospital in Madhya Pradesh dist Burhanpur - Apple + hospital but it seems no one aware of this scheme as I enquired with hospital staff.
staff nurse 5 years expierence working in icu
KAFI ACHHI YOJAN HAI MAI BHI JOIN KARNA CHATA HU PLEAS MERA EMAIL ID PER REPLY DE DIJIYEGA
Pls give us whole details for ayushman bharat with their tollfree number
me bhi ayushman mitra ka course krna chahta hu sir kese hoga ..frome kese apply kre ????
Sir ayushman bharat ka form online kab hoga
Its customer support number not correct. Someone pickup call and talks very rudely. I dial this number, he pick up call and say i don't anything about that. After that i visit official website to get customer number, they all numbers are not valid. So... what is this?
hello sir Mai jharkhand se hu Mai v is yujna ka hissa bana chahti hu
hello sir Mai jharkhand se hu Mai v is yujna Mai hissa Lena chahti hu
main es yojna ka ek karykarta banana chahta hun
i am interested to apply the post of ayushman mitra at ASSAM , DARRANG,PIN: 784146
MERA NAME HE YA NHI
Hai N Ramu Andhra Pradesh ayushmanmithra job o line notification appudu veystharu
Fantastic scheme for middleclass people. Which date application will be release.we want apply that.
sir pardhan mantri jan arogya yojna me kese jude sir please hel me
Mai pm modi ji ko support karta hu isake liye it is very nice youjana
i ma salman khan
sir date kab aayega form daalne ka ...
Do AyushmanBharat covers Cataract surgery ?
Pradhan Mantri Jan Arogya Yojana (PM-JAY) covers Cataract surgery ?
Kumarsumit8876@gmail.com
Kumarsumit8876@gmail.com
How I can apply ayusman mitra post ?kindly reply me.
jinka list me name nahi hai, unke liye kya
Dear Sir,
How can i apply for the Pradhan mantri jan arogya yojana. What is the website i want to see. please guide me.
आयुश्मान भारत योजना केंद्र सरकार प्रधान मंत्री नरेंद्र मोदी द्व्रा लांच की गयी एक सब्से अच्छी योजना है । इस योजना के द्व्रा हर गरीब को 5लाख तक का इलाज निशुल्क मिलेगा आज तक भाजपा सरकार के अलावा इतना अच्छा कदम नही लागु किया । मैं अनुज पटेल और मेरे बाबा बीपी पटेल भाजपा सरकार की बहुत बहुत स सरहाना करते है ।
प्रेशक -
अनुज पटेल class - 2 k. k. s. विधालय बीसलपुर ग्राम - अकबर गंज सिमरा पोस्ट - खास तहसील - बीसलपुर जिला - पीलीभीत
sir distric muzaffar bihar se hai ayusmanmitr me kyse apply karenge
How to get health card from csc
Ayusman bharat health scream kob start hoga,iam aggry this scream.please help me.
AYUSHYAMAN BHARAT KA REGISTRATION KAHA KARNA HOGA
Sir: Mai Gareeb pariwar se Bilom karta hu, aur Hum garibo ka koi Sunwai nahi hai, Kyunki Jitna Sarkari Yojana Gareebo ke liye Aati hai AK bhi Yojana Gareeb Ko nahi Milta hai,ye Sarkari Yojana jinke paas Paisa hai unhi Ko Milta hai
ham madhyam varg ke log hi sarkari yojna ka faida nahi le pate yojna sirf paise valoke liye hai ya garib ke liye ham madhaym varg kaha jai ye bhi bata de sarkar
MODI SARKAR NE MERE JAISE ANEK GAREEB PARIWARON KE LIYE KOI FAYDE WALI SCHEME NAHI DEE HAI MODI NE KAHA THA SABKE KHATE ME 15 15 LAKH RS. DALOONGA AUR AAJ TAK 15 PAISE BHI KHATE MEIN NAHI AAYE MODI SARKAR BILKUL BAKWAAS SARKAR
Suresh Chand Gupta, if you belong to BPL family, then you have received health insurance scheme worth Rs. 5 lakh per family per year. Modi sarkar is making arrangement of rest Rs. 10 lakh to complete your payment of Rs. 15 lakh...
rely
ausaman bharat youjna is very poor and back bord parson is so improv our life and ourfutacher in daly life
so i proudof our govement .jai ho india.
jai hind
kya mea registration
AYUSHYAMAN BHARAT KA REGISTRATION KAHA KARNA HOGA
how to surch the empanellment hospital
please reply
m bhi join krna chata hu kafi achha h ye yojna
Dear sir,
I am from Mumbai (Andheri) PIN code 400069
DOB 19/06/1959
i had CABG in 2009
is am i eligible for PMJAY (Ayushman Bharat)
If yes pl. inform me my name in above list
Regards
suresh bhaskar, please provide us your ration card number or RSBY URN or mobile number registered or personal details such as name / father's name/ mother's name / spouse name / age / district / village / pincode. If you want a quick response, please provide us your ration card number.
Best yojana
I want to join this Yojana.
I WANT TO JOIN THIS YOJANA.
i want join this yojna
i want to know about this program
Indeed a great step by our PM. This is worlds biggest health insurance scheme run by state. Very detailed information...Thank you
no comment
How can I enroll me and my wife in this Ayushman Bharat Yojana.
How I can reply me
Plz call? 8210428910
Vill+post saknara p s madhabdihi dist purbabardhaman
Virendra thakur
how can i do applygujarat,mehsana
ayushman bhart me dusre ke rashan me kisi our ka name khul raha hai. kya yahi ayushman bhart hai .
Es yojana me kaise from online hoga sir aur apne family card kaise Banega plz plz jara bata dijiyega
Mr. Ramharankh, check your name in the PMJAY beneficiaries list at mera.pmjay.gov.in. If you are eligible, then check the empanelled hospitals list at pmjay.gov.in. Then go to any of the empanelled hospital, there would be an arogya mitra present at the hospital who would assist you in making family cards. It is hereby clarified that for the 1st time treatment, you can take any ID proof to the hospital.
Es yojana me kaise from online hoga sir aur apne family card kaise Banega plz plz jara bata dijiyega aur mai bhi eska course karna chahta hu aur es time mai biology se reading kar raha hu esaka reply mere email id par jarur dijiyega plz sir
I have not received any information of Ayushayaman yojna please do the needful at the earliest
Thanks
Ashvin Gokani
Jamnagar
9427281081
Ayushman Bharat Yojana is also known as Pradhan Mantri Jan Arogya Yojana (PMJAY) - Check Details. To find name in the list of beneficiaries, click at PMJAY beneficiary list
Kaise rajestation kare
Mr. Kameshwar, Ayushman Bharat Yojana across India is an eligibility based scheme and there is no enrollment / registration / application process. Directly check your name at mera.pmjay.gov.in. In case you are from Uttarakhand, only then you can apply for online registration under PM Jan Arogya Yojana.
I'm interested
mujhe ayushman mitr ka from bharna hai
m bihar begusarai se hu
NO COMMENT
Sir B.A pass hoon sir job milega sir grib ghar ka student hoon sir
how i can know my name is present in ayusman bharat
Where's my name in list
This yojna is only in benefit of insurance company and limited empanelled hospital becz govt is not giving empanelment to fresh hospitals
Dear Sir ,
My Name is in Ayushman Bharat Scheme or not plz Replay Sir .
My Mobile No. 9616467004
My Aadhar No. 6414 4866 6080
My Name is in Ayushman Bharat Scheme or not plz Replay Sir .
dhage.shivaji17@gmail.com
Respected sir,
As I am on dialysis age 38 with APL card in Maharashtra state. Is it possible for me to get benefit of ayushman Bharat scheme.please state any way from this condition.
Bahadurgarh
I m pregnant. Sir mai koun se hospital me ja k delivery karahi.nagpur me
aap ke nagpur area me jis bhi hospital ka naam ayushman bharat yojana ki hospital list me to vahi pr jana chara
When it can be start availing if i am eligible
how to register complaint regarding hospital was not accepting this insurance.
any mail id is available for registering complaints. please share Email ID.
If the hospital is in the list of Ayushman Bharat Empaneled hospitals, it must accept else, contact the Ayushman Bharat Helpline
i am widow of 89 yrs.old but my name is not found in eligible list to enrolled under Ayushman bharat health insurance by p.m. modi my ration card no is in name of my late husband shamji waghela my mobile no is in name of my son Mahesh 9323783079 i am residing in mumbai 400002 maharashtra state in eligible list it show records not found ,now how can i enrolled myself for this govt.scheme?
You need to contact the nearest Ayushman Mitra Kendra or civil hospital if there is a way of enrolling into the scheme
sir i m interested to this scheme as a csc how to open csc centre?
Mobile 9199673630
Khaniydana julaa supree m p
I KAMAL HIRAWAT FROM SILIGURI WESTBENGAL, WANT TO MAKE MY AND MY FAMILY MEMBERS CARD OF "Pradhan Mantri Jan Arogya Yojana (PMJAY)". SO KINDLY HELP ME TO PROCESS THE FORMAT AS SOON AS POSSIBLE
At-Malipadi, post-bankamuhan, dist-bhadrak
Mera name prabhash jha d.o.b_5/8/1991 Mera ayushman Bharat me hi please sir
If any Impaneled Hospital of Ayushman Bharat Yojna is not accepting the PMJAY Golden Crad you can register complaint against them at https://cgrms.pmjay.gov.in/Website/OnLineRegisterComplaint.aspx site.
I want about eyes hospital under ayushman bharat
If any Empaneled Hospital of Ayushman Bharat Yojna is not accepting the PMJAY Golden Crad you can register complaint against them at https://cgrms.pmjay.gov.in/Website/OnLineRegisterComplaint.aspx site.
Hello, this weekend is nice designed for me, because this moment i am reading this impressive informative post here
at my house.
This plan is good. But the economic census of 2011 is not correct.The beneficiary does not benefit from this plan.2011 that the economic census was done by the teacher who showed negligence.
And did not play your responsibility fully sincerely.Because of which the real beneficiary was deprived of this wonderful scheme Government should think this.
Maheshbhai Solanki(Gujarat)
Our family is not yet covered under PMJAY scheme.Pl inform how I can get benefits under the scheme.
I love
arbindsarma1234@gmail.com
difficulty in empanelment of new nhospital,240 medical enclave Amritsar punjab
Sir meri qualifications d pharma(diploma in pharmacy)h.ayusman Bharat yojna m job kese milegi .from Haridwar Uttarakhand.thankyou.
I accept to the job
Am interested in this job
12 pass out
(DEO) Deploma
Basic computer
Please give me
Job sir
Thank you sir.
pleas a
gayanbaghela99@gmail.com Jaisalmer Rajasthan.com
sir please mera bhi jan Arogya yojana me list jari karne ki kripa karne kyoki mai ek berojgar v meri wife ki tabiyat akhsar kharab rahti hai please sir
sir we want empanled our hospital . guid us thanks
नागरिकों को 'नियंत्रण से परे' बीमारी के उपचार में अत्यधिक महत्वपूर्ण यह योजना है,किन्तु निजी क्षेत्र के उच्च चिकित्सा संस्थानों व सार्वजनिक उच्च चिकित्सा संस्थानों की अरुचि के कारण इसका लाभ न्यूनतम है।
अधिकांश लाभार्थी परिवार गरीब व अशिक्षित है जो जागरूकता के अभाव व त्वरित चिकित्सा सहायता की आवश्यकता से ,आयुष्मान कार्ड धारी होने के बावजूद भी धन-धरा बेंचकर या कर्ज लेकर सामान्य इलाज करा रहे हैं।
हर ग्राम पंचायत पर नियुक्त csc के सेवा प्रदाताओं के माध्यम से इसका प्रसार व 'आयुष्मान मित्र' के रूप में csc को चयनित कर निश्चित न्यूनतम मासिक सहायता राशि के साथ प्रोत्साहन राशि देकर इस महत्वाकांछि योजना का प्रसार किया जा सकता है।
राजेन्द्र सिंह
Bhind
mere ma ke ilaj ke liye muze PMJAJ ka card mila nahi hey
muze card ki bahut jarurat hay
please muze form bhej do
Muze mere maa ke Ilaj ke liye PMJAY ka Form Mila nahi hey
please muze wo form bhej do mere maa ka ialaj karana jaruri hey
sir please mera bhi jan Arogya yojana me list jari karne ki kripa karne kyoki meri ma ki tabbiyat khrab hey use cancer huwa hey isliye mera nam hona jaruri hey mere pas itane ruppye nahi hey mey iska ilaj kar saku please
Vipo mokalwash
Mokalwas near darmshala
Vipo mokalwas near darmshala
I am interested Ayushman Mitra this post How to apply
Narayan Barman
Villege.ruidanga
Po.ruidanga atpukuri nayahat
Ps.ghoksadanga
Dist.coochbehar
Pine.735211
State Westbengal
I WANT TO JOIN
Namaste
It's great sckeam for India. I interested
It's a great sckeam for India. I interested.
skrao7861432@gmail.com
kya sir mai es yojna ka labh le sakta hu
Happy
nice yojna
Nice yojna
VILL&PosT_TANDIWANDistHardoiUttarPradeshModileNo9582036765
DEAR SIR
IN THE AYUSMAN YOJNA CARD OUR FAMILY NAME ARE WRONG.
PLS TELL ME HOW THESE NAME CAN BE CURRECT.
Me bhi 1 grib pariwar se hu mere masik salery 10000 hai or mujhe bhi modi ji ki is yojna me samil hona pr mera kisi bhi hangame naam nhi aaya mujhe aayush maan bharat sceam me inrollment ke liye kya krna pdega
मेरा आयुष्मान कार्ड में पूरा परिवार का नाम गलत है
कैसे इसको सुधार आ जाएगा आप श्रीमान से अनुरोध है कि इसके बारे में जानकारी दें...!!
How to register in pradhan mantri jan aarogya yojana?
Pl check my name in Ayushman Bharat Yojna
Name : Bipin Father name : Shankarlal other Name : Manguben
Mobile No : 9327000842 , Pin : 382006
sultanpur pmjay hosipital list
DEEPAK GUPTA
VILLEGE JAGDISHPUR MISIRPUR
Lambhua
distt sultanpur up
Rajurawat lodhi puram agra road aligarh
Dear sir/Madam.
Humare gaav me aayushmaan ke card nhi ban rhe hai kripya karke humarr gaav me card bnane ki suvidha pardan ki jaye humara gaav haryana k sirsa jila me hai humare gaav ka naam h shahidanwali (88)
Lakhan yadav
Lakhan yadav
My problem deaceg Parkinson
arogya mitra
I have passed ssc examination & 3 years diploma in mechanical engineering. Can I get aarogya Mitra job.
Aarogya mitra
Ayusman bharat (medical benifit kob milega), kolkata West Bengal
Thank you so much sarkari yojna team for this efforts of providing very essential and informative information in a very simple and detailed way.
I appreciate your work.
I want to see All pm yojna .
MY AAYUSHMAN CARD IS NOT PROVIDED ME..NITER MY MOTHER OR FATHER.HE IS OLD AGE PLS PROVIDE MY FATHER MOTHER AAYUSHMAN CARD..
D-324 BAHAGT SINGH COLONY BALLBGARH FARIADABAD HARYANA 121004
Very Good
Have a good day
Sir hamare ghar me am Marin bimar he isleye hame ayushman Bharat card ki mang kar rhe hospital me to sir. Secc no nhi hone ke Karan card nhi bana
sehabis membaca blog iini saya bisa mendeskripsikan bahwa penulisan yang di jelaskan bermanfaat.
adnankhan76181@gmail.com
Arjun Sigha dob/ 11/8/1987 s/o SURAJ SINGH
Teacher colony devi road mainpuri uttar pradesh
Pn 205001
Rangpatti ward4 mangarwara p.s shreenagar via kumarkhand distc madhepura state Bihar pin code 852112
Sujit kumar so rajit ram patel Patel 68 jay mhadevnagar pandesrs bamroli City gujrat 394221
Sir can I register in your yojna I am at home for last 13 year & depended upon father & brother pH 8087268680 thanks
Natnachapravadjahmedavad Gujarat India
Natnachapravadjahmedavad
My name is enrolled in ATAL AMRIT ABHIYAN on dt.14.July 2017.can I get the benefits of ayushman bharat.plz acknowledge.
Sir, I would like to know the validity status of my PMJAY # P1TQOLS8Z.
You can track your Ayushman Bharat - PMJAY status at https://mera.pmjay.gov.in/search/login
'
;olki
IN AHMEDABAD GUJARAT WHERE CAN I DO THIS Ayushman Mitra Training ??
Gaytri Verma Lucknow se likh rahi hoon Mera aaj Tak Ayushman card nahin Ban Paya hai atah aap se nivedan hai ki mera Ayushman card banane ki meri madad Karen mujhe iska Labh prapt ho se Banega aata aap meri madad karvai a Lucknow Alambagh Bheem Nagar
Mera abhi Ayushman card nahin Ban Pa raha hai aur hamen Koi uski jankari bhi nahin de raha hai aur humko sab idhar udhar Dora a rahe hain sare Adhikari aap se nivedan hai mera Ayushman card banwane Meri madad Karen main bhi Nagar Alambagh Lucknow se likh rahi hoon mera naam Gayatri Verma hai
Firstly check if your name is present in the Ayushman Bharat Yojana list through the link - https://mera.pmjay.gov.in/search/. If your name is present in this PMJAY list, you can take a printout of the name presence which will be the proof that you are eligible for cashless treatment. Then your Ayushman Bharat Yojana Card would be made at the nearest govt. hospital.
kaise apply hoga plz help me
आयुष्मान भारत कार्ड में भी बनवाना है
MANGESH KANAKE POST APLY COMPUTER OPERATOR AT LAKHAPUR POST NANDEPER TQ MAREGAON WANI DIST YAVATMAL 445304 MOB.
Devji bbariya
Fibroadenoma breast
Aahok verma chillawan.9519434103.8840384975
Mai berojgar baitha hu gar pe gar ka kharchha bhi nhi chal pa rha hai
sir mera aayushman card banane ke karpa kare
Assam list
Sir,
How to know my name in PMJAY arogiya list. My mobile no 9847752777, Aadhar no.4604 8694 4536. If name available give me H H ID No.
Thanks,
Kuruvilla Koshy
You can check your name in PMJAY List through the link - https://mera.pmjay.gov.in/search/login
AUYSHMAN ID CEREATE