Tamil Nadu government is inviting TN Chief Minister Comprehensive Health Insurance Scheme 2026 Application Form at www.cmchistn.com. All the people who have been enrolled in Chief Minister's Comprehensive Health Insurance Scheme can now perform CMCHIS Card download from the official website. In this article, we will tell you about eligibility criteria, how to enroll process, link aadhar with URN, perform member search, check e-card instructions, find member ID, check benefits, treatment package rates, hospital list etc.
Chief Minister MK Stalin on his first day in power has included COVID-19 treatment under TN Chief Minister Comprehensive Health Insurance Scheme 2026. CM Stalin mentioned that the Tamil Nadu state govt. will bear the entire cost of Coronavirus treatment as it is now covered in CMCHIS. Here we read the MK Stalin Decisions announced on first day after coming to power in Tamilnadu.
What is TN Chief Minister Comprehensive Health Insurance Scheme 2026
Chief Minister Comprehensive Health Insurance Scheme launched by the Government of Tamil Nadu through United India Insurance Company Ltd, a Public Sector Insurance Company headquartered at (Chennai). The scheme now covers 1.57 crore families including migrant workers and undocumented orphans. Tamilnadu CMCHIS provides quality health care to the eligible persons through empanelled government and private hospitals. This scheme aims to reduce the financial hardship to the enrolled families and move towards universal health coverage by effectively linking with public health system.
The CM Comprehensive Health Insurance Scheme provides coverage for meeting all expenses relating to hospitalization of beneficiary as defined in the scope of the scheme. In this article, we will tell you about the complete details of the Tamil Nadu CM Comprehensive Health Insurance Scheme.
How to Enroll for CM Comprehensive Health Insurance Scheme in Tamil Nadu
Any eligible person wanted to enroll for the CM Comprehensive Health Insurance Scheme, following steps needs to be followed:-
- Please obtain income certificate for the family from the VAO.
- The Family head/member should carry the original ration card with Xerox copy along with income certificate to the district kiosk.
- The DK operator, after verification of the documents, will enroll the member by capturing the demographic and bio metric details.
- After capturing the members photograph, ecard will be generated and issued to the beneficiary.
Check Enrollment Process in Tamil through the link - http://www.cmchistn.com/howToEnroltam.pdf
Eligibility Criteria under Tamilnadu Chief Minister's Comprehensive Health Insurance Scheme
The eligibility criteria to avail Chief Minister’s Comprehensive Health Insurance Scheme is given here.
- This scheme is for the resident of Tamilnadu whose name is present in the Family card. CMCHIS is applicable to those whose annual income is less than Rs. 72,000 per annum.
- For being eligible for benefits under the scheme, it is sufficient to produce family card and Income Certificate by the VAO/Revenue authorities along with the self declaration of the head of the concerned family.
- “Family” includes the eligible member, and the members of his or her Family as detailed here - (i) Legal spouse of the eligible person (ii) Children of the eligible person (iii) Dependent parents of the eligible person provided that if any person, in any of the categories at (i), (ii) or (iii) above, finds place in the family card then it shall be presumed that the person is member of the Family and no further confirmation would be required.
- Srilankan refugees in the camps are also eligible without any Income limit.
- Migrants from other states can also join this CMCHIS based on the request letter along with a list of Eligible member’s from labour department, provided they have resided for more than six months in the state as certified by suitable authority.
- Orphans residing in any registered/unregistered organization can be given a single card. This also includes the rescued girlchildren and any other person defined as orphan by the government.
Detailed eligibility criteria and other information about Chief Minister Comprehensive Health Insurance Scheme is available through the link given here - http://www.cmchistn.com/eligibility_en.php
How to Link Aadhar With URN
- The existing beneficiary shall open this tab "CMCHIS Online".
- In the given slot please enter your 22 digit URN.
- Click the check box for acceptance to enter your aadhar number.
- Click the Enroll Now button and the user will be redirected to a page where the user needs to select the Family member and enter their Aadhar number and mobile number in the box provided.
- After entering the aadhar number and your mobile number, click submit button. The user will receive a OTP in the given mobile number. Enter that OTP in the box provided. You will receive a message as “Your Aadhar number registered successfully”.
- If your Aadhar number is already linked with URN, you will receive a message as “Already Registered”.
Check How to Enroll Aadhar with URN in Tamil through the link - http://www.cmchistn.com/howToEnrolAdharURNtam.pdf
Member Search / E-Card Instructions
- Firstly visit the official website at http://www.cmchistn.com/
- At the homepage, scroll over the "Enrollment" tab, then at Member Search / E-Card and then click at the "Instructions" option.
- Click the direct link - http://www.cmchistn.com/memInstr.php
- In the opened window, click at the "Go to Member Search Page" as shown below:-

- Next, the page to perform member search / e-card under CMCHIS scheme will appear as shown below:-
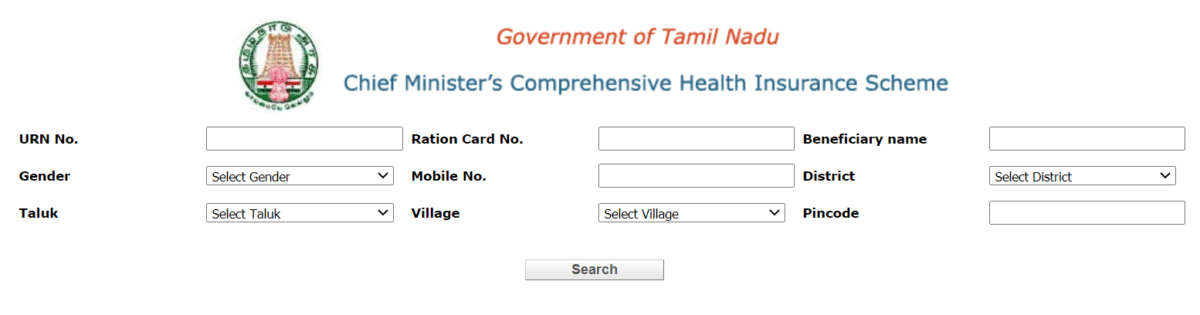
- Here applicants can enter URN, Ration card number, Beneficiary Name, gender, mobile number, district, taluk, village, Pincode and then click at the "Search" button to perform member search / e-card under Chief Minister Comprehensive Health Insurance Scheme.
Member ID under Chief Minister Comprehensive Health Insurance Scheme
- Firstly visit the official website at http://www.cmchistn.com/
- At the homepage, scroll over the "Enrollment" tab, then at Member ID
- Then the page to search URN under CM Comprehensive Health Insurance Scheme will appear as below:-
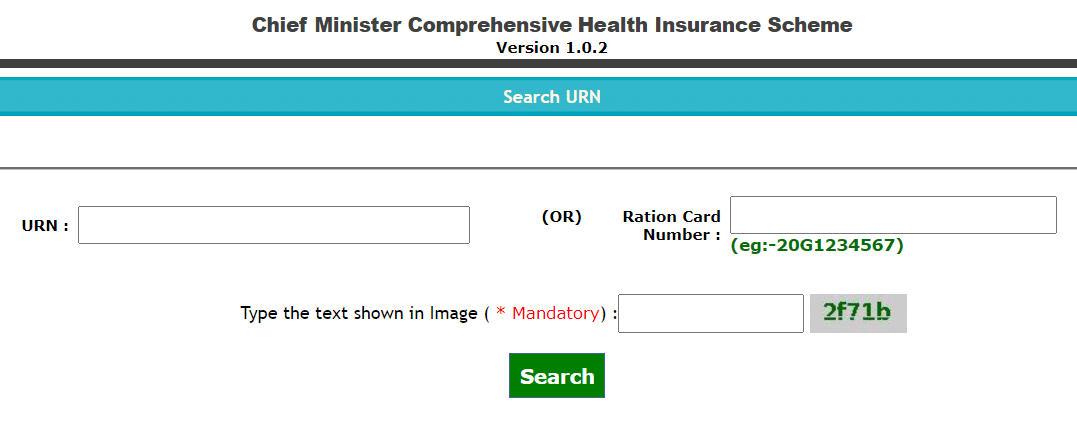
Here applicants can enter URN or Ration Card number and then hit at "Search" button to find CMCHIS Member ID.
Benefits of CM Comprehensive Health Insurance Scheme
The CMCHIS seeks to provide cashless hospitalization facility for certain specified ailments/ procedures. The scheme provides coverage up to Rs. 5 lakh per family per year on a floater basis for the ailments and procedures covered under CM Comprehensive Health Insurance Scheme. List of Procedures is also available in the CMCHISTN website. The scheme also grants cover for Follow-up Treatment as listed under Annexure "E" in addition to any other specific procedures listed in Annexure C and Diagnostic procedures listed under Annexure "F".
Chief Minster's Comprehensive Health Insurance Scheme has broadened its coverage and also included 321 more medical procedures. Along with United India Insurance Company, the Chief Minster's Comprehensive Health Insurance Scheme renewed on 10th January 2017. The scheme will have more than 1,100 treatment procedures including the coverage of congenital anomalies. The government renewed the contract for four-year terms with an annual premium payment of Rs. 1,069 crores.
As per the information from Public Health and Preventive Medicine department, the government is paying Rs. 699 on per family basis while earlier, the amount was Rs. 497. The departments have the responsibility for implementing the scheme properly.
Treatment Package Rates under CM Comprehensive Health Insurance Scheme
Tamil Nadu State Health Insurance Scheme will be covering the treatments and procedures including, heart and lung transplants, cochlear implant, bone marrow transport, radiation therapy, surgical oncology. For the first time in India, it is the first scheme to cover the cover bariatric surgery for the morbidly obese. The detailed list of treatment package rates covered under the scheme are available at http://www.cmchistn.com/prate.php
The coverage amount under the scheme has been increased from Rs. 1.5 lacs to Rs. 2.0 lacs and then to Rs. 5 lakh for surgical procedures. It is the first attempt of Tamil Nadu state government towards providing a health insurance cover to migrant workers and orphans. The scheme was not benefiting this category from a long time due to the lack of documentation, address and residence proof. With some amendments and modification in State Health Insurance Scheme, the government hopes to reach those workers and their children who have no or less documents.
Tamil Nadu Chief Minister Comprehensive Health Insurance Scheme Hospital List
- Firstly visit the official website at http://www.cmchistn.com/
- At the homepage, scroll over the "Empanelment" tab, then at "Empanelled Hospital List" and then click at "EDC Hospital" link
- Afterwards, the complete Tamil Nadu Chief Minister Comprehensive Health Insurance Scheme Hospital List will appear as shown below:-
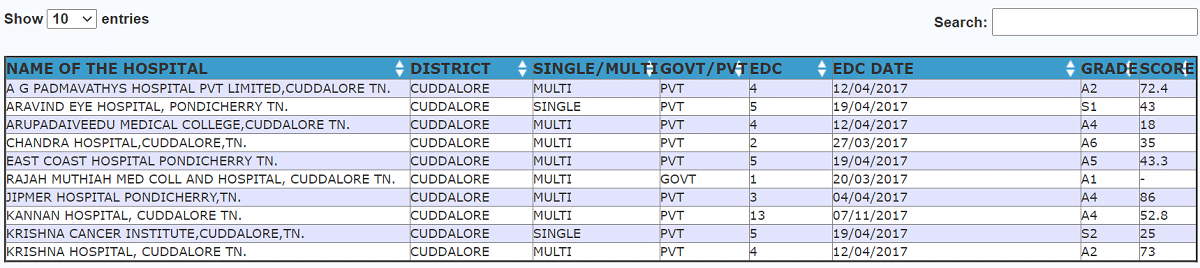
People must check the name of the hospital in the empanelled hospitals list to get free treatment under CMCHIS.
Tamilnadu CM MK Stalin Schemes Announcement Regarding CMCHIS
At the first day in office, Tamilnadu CM signed five important files.
- Rs. 4000 TN Covid Relief Scheme: The first was to provide financial assistance of Rs. 4,000 as COVID relief to each family (2.07 crore Rice Ration Card Holders). The amount of Rs. 4000 would be paid in 2 installments and first installment of COVID Relief Package would be transferred in the month May 2026. This scheme will aid citizens affected due to the pandemic and help them with their livelihood. To implement that, the Chief Minister has signed the order to provide the first installment of Rs 2,000 in May itself at Rs 4,153.69 crore, covering 2,07,67,000 ration card holders,
- Reduction in Milk Price of State Run Aavin: Stalin ordered slashing the price of Aavin milk by Rs. 3 per litre from 16 May 2026.
- Free Travel Scheme for Women / Girls: Free travel for working women and girls pursuing higher education on board government buses (ordinary fare) across the state. Women can travel free of cost in all ordinary fare city buses operated by State transport corporation from 8 May 2026 onwards and the government has allocated a sum of Rs. 1,200 crore as subsidy for this purpose.
- 100 Days Complaint Redressal: CM ordered to implement a grievances redressal mechanism to resolve issues within 100 days. CM Stalin has approved constituting an IAS officer-headed department to implement the "Chief Minister in Your Constituency Scheme" to fulfill another assurance of redressing people's issues within 100 days of taking over, on petitions received by him ahead of the polls as DMK chief.
- Free COVID-19 Treatment in CMCHIS: CM also ordered that the State government will bear the cost of Covid-19 treatment as it is now covered under CM Comprehensive Health Insurance scheme. Stalin announced bringing COVID-19 treatment in private hospitals under a government insurance scheme, to provide succour to such people.
Enrolled Beneficiaries Count in Tamil Nadu CM Comprehensive Health Insurance Scheme
Helpline Number of CMCHIS
A 24 hour Call Centre has been set up at CMCHISTN Project Office with sufficient manpower with toll free help line. The Toll Free Number is 1800 425 3993. The Toll Free Line is competent to answer the query in Tamil.


Sir. My home loan
What is the meaning of PHH in smart card?
மதிப்புக்குறிய ஐயா.
என் பெயர் விஜய், நான் என் மனைவி மற்றும் என் மகன் 4வயது இப்போது வேலை இல்லாமல் மிக அவதி படுகிரோம், எங்களுக்கு இலவச வீடு பெற உதவவும்
cell 7010298588
Nice to meet
We have Tamil Nadu Chief Minister Comprehensive Health Insurance Card. On going the list of Eye Hospital under Tamilnadu Government
Chief Minister Comprehensive Health Centre Aravind Eye Hospital at Tuticorin is not recommended. If Eye treatment is done at Tuticorin
kindly inform us whether the medical expenses is to be imbursed on submission of necessary documents like Bill, etc.